LIVER AXIS
Why Liver Disease May Begin in the Gut
What if one of the most common liver conditions today isn't just about fat — but about signals coming from the gut?
Over the past decade, liver disease has quietly become one of the most common metabolic conditions worldwide. But recent research is shifting the conversation in a profound way:
👉 The liver may not be the true starting point.
Instead, scientists are now focusing on what is called the gut–liver axis — a direct biological connection between the digestive system and the liver that is now considered central to how liver dysfunction develops.
(Frontiers in Microbiology, 2025; Nature Reviews Gastroenterology & Hepatology, recent updates)
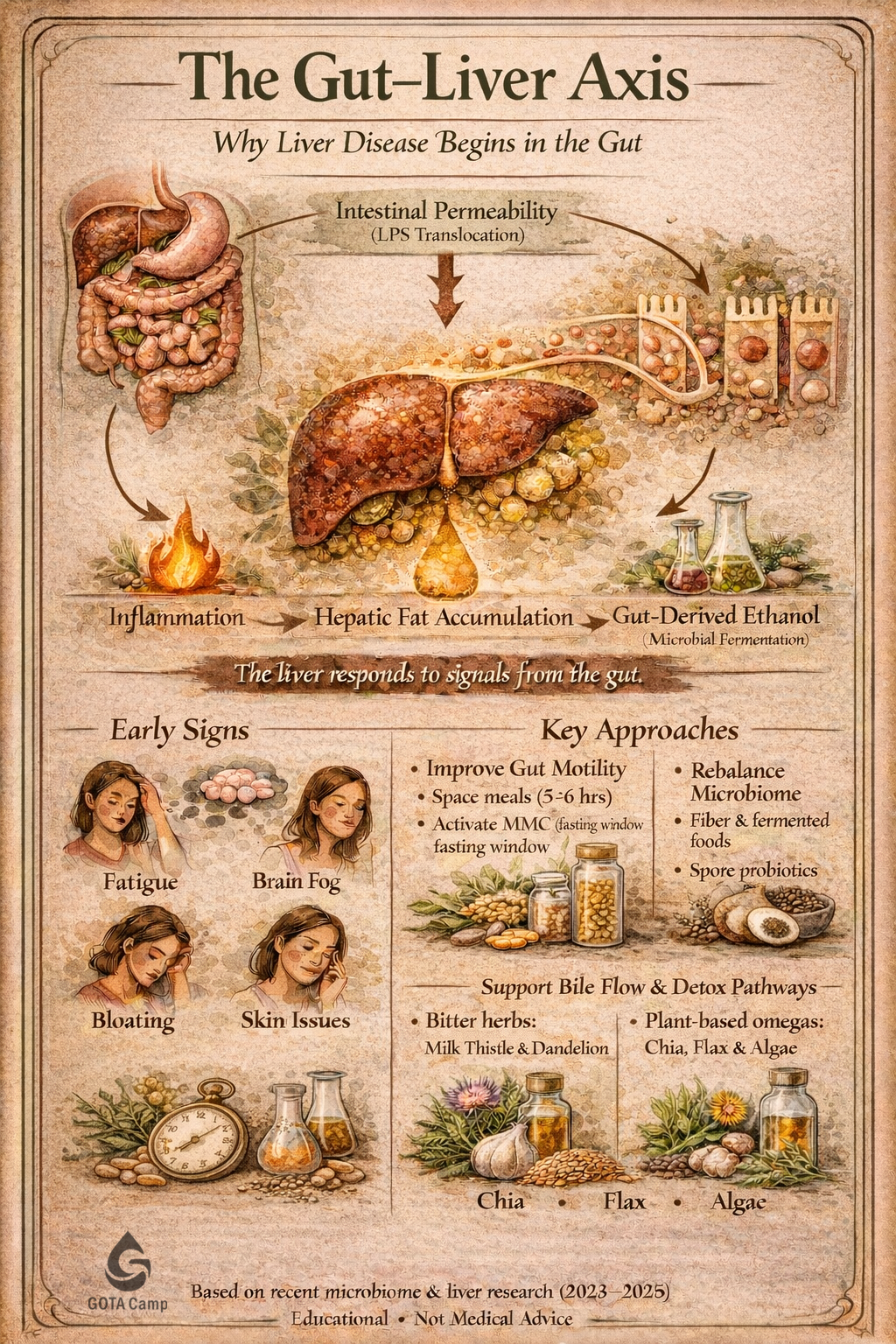
A Direct Connection: The Gut Talks to the Liver
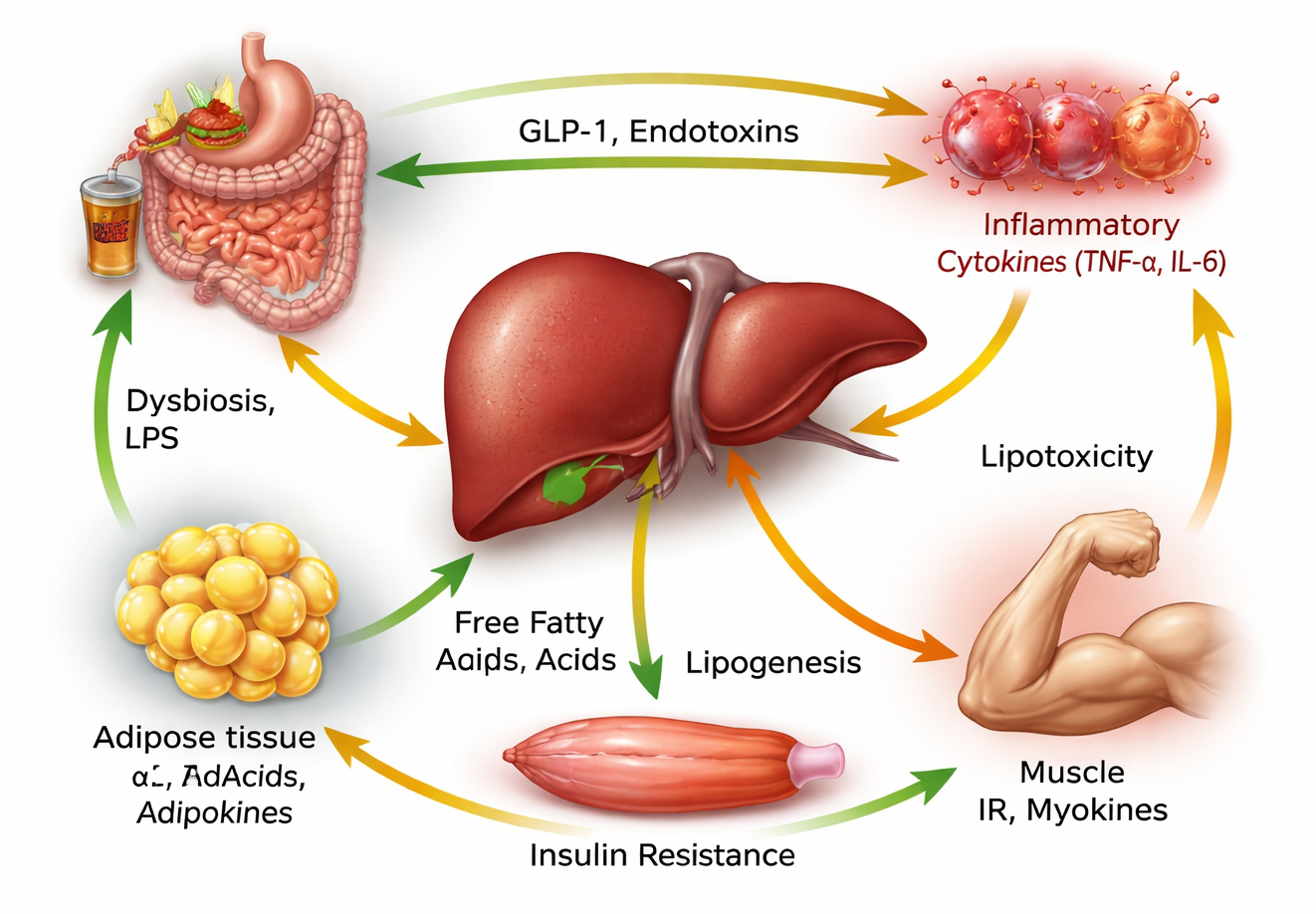
'The liver receives nearly 70% of its blood supply directly from the gut through the portal vein.
This means that everything absorbed in the intestines — nutrients, microbial metabolites, and toxins — is delivered straight to the liver. When the gut is balanced, this system supports metabolism and detoxification. But when the microbiome becomes disrupted, the signals reaching the liver begin to change.
Emerging research shows that:
microbial imbalances can influence liver fat accumulation
gut-derived toxins can trigger liver inflammation
microbiome activity can alter insulin sensitivity and metabolic signaling
In this sense, the liver is constantly responding to the environment created in the gut. (Frontiers in Microbiology, 2025; Hepatology Communications, 2024)
A New Name, A New Understanding
One of the most important recent changes in liver research is the shift in terminology:
👉 Non-alcoholic fatty liver disease (NAFLD) is now being redefined as Metabolic Dysfunction–Associated Steatotic Liver Disease (MASLD)
This reflects a deeper understanding: Liver disease is not simply about fat — it is about metabolic dysfunction, inflammation, and systemic imbalance.
Importantly, this condition is now being identified in:
individuals who are not overweight
people who appear metabolically “healthy”
those without obvious symptoms
This helps explain why liver dysfunction can develop silently and go unnoticed for years. (Global consensus statement on MASLD, 2023; ongoing literature updates through 2025)
When the Gut Barrier Breaks
The intestinal lining acts as a selective barrier — allowing nutrients in while keeping harmful compounds out. However, when the microbiome becomes imbalanced, this barrier can weaken. This allows bacterial components — particularly lipopolysaccharides (LPS) — to pass into circulation and travel directly to the liver.
Once in the liver, these compounds can:
activate immune cells
trigger inflammatory pathways
promote fat accumulation within liver cells
This process is now recognized as one of the key drivers of liver inflammation and disease progression (Frontiers in Microbiology, 2025; Nature Reviews Gastroenterology & Hepatology)
An Unexpected Discovery: “Internal Alcohol”
One of the more surprising findings in recent research is that certain gut microbes can produce ethanol inside the body. These microbes ferment carbohydrates and generate alcohol as a byproduct — a process that can occur entirely within the intestine.
In some individuals, this may contribute to:
liver stress
inflammation
metabolic disruption
Even in the absence of alcohol consumption. This emerging concept is helping researchers better understand why some individuals develop liver disease without traditional risk factors. (Yuan et al., Cell Metabolism; Frontiers in Cellular and Infection Microbiology, 2023–2025)
A Deeper Layer: Fermentation, Motility, and Modern Eating Patterns
Ethanol production in the gut is not random — it depends on the internal environment of the digestive system. Research shows that microbial fermentation increases when:
fermentable substrates (especially carbohydrates) are abundant
microbial balance is disrupted
intestinal transit is altered
One key factor is gut motility. The digestive system relies on rhythmic cleansing waves — known as the migrating motor complex (MMC) — which occur during fasting periods. These waves help:
clear residual food
regulate microbial populations
prevent excessive fermentation in the small intestine
However, when eating occurs continuously throughout the day, these cleansing cycles may be reduced. This can create a more favorable environment for microbial fermentation.
While research is still evolving, current evidence suggests that conditions that prolong digestion or reduce motility may favor fermentation pathways, including those that produce ethanol. (Physiology of the Migrating Motor Complex; SIBO and motility literature, 2023–2025 reviews)
Why You May Not Feel It
One of the most important aspects of liver health is this: Liver dysfunction often develops without clear symptoms. Early changes may not produce pain or obvious warning signs. Instead, subtle patterns may appear, such as:
fatigue or low energy
brain fog
mild digestive discomfort
skin imbalances
difficulty with metabolic regulation
Because these symptoms are nonspecific, liver stress is often overlooked until it progresses. (Hepatology reviews on early-stage MASLD, 2024)
The Good News: The System Can Rebalance
The same interconnected system that contributes to dysfunction also offers an opportunity for recovery. Because the gut and liver are closely linked, supporting one can positively influence the other.
Research shows that targeted changes can:
improve microbial balance
reduce inflammatory signaling
support metabolic function
decrease liver fat accumulation
Often within weeks to months. (Journal of Hepatology, lifestyle intervention studies; 2024 updates)
Supporting the Gut – Liver Axis
Key strategies that support this system include:
allowing adequate time between meals to support digestive cycles
supporting microbial diversity through whole, fiber-rich foods
maintaining healthy gut motility
supporting digestion and bile flow
reducing factors that disrupt the microbiome
Foods that are particularly supportive include:
leafy greens
cruciferous vegetables
legumes
berries
herbs such as dandelion and milk thistle
These help create an internal environment that supports both microbial balance and liver resilience.
5 Signs the Gut–Liver Axis May Be Imbalanced
Because this is a connected system, symptoms may appear across multiple areas:
Persistent bloating or digestive discomfort
Brain fog or difficulty concentrating
Skin imbalances
Fatigue that does not improve with rest
Difficulty losing weight despite healthy habits
While these signs are not diagnostic, they may indicate that the system would benefit from support.
Key Takeaways
The gut–liver axis plays a central role in liver health
Liver disease is increasingly linked to microbial and metabolic factors
Gut-derived toxins and fermentation byproducts can influence liver function
Certain microbes can produce ethanol inside the body, contributing to liver stress
Digestive patterns and gut motility may influence microbial activity
The system can recover when properly supported
Understanding this connection may change how we approach prevention and long-term health.